Obstacles to healthy living – such as not getting enough sleep or feeling anxious – can take a serious toll on anyone if these experiences occur over a prolonged period. For people with substance use disorders, these issues can complicate the recovery process, and may have even been the catalyst for their substance use in the first place. The National Institute on Drug Abuse has stated that of the over 20 million adults with substance abuse disorders, nearly 38% also suffer from mental illnesses. This condition of battling two disorders is known as dual diagnosis.
The Challenges of Living with a Dual Diagnosis
Co-occurring mental health issues can be a tremendous burden for people in early addiction recovery and are not only distracting but debilitating. At Mountainside, we strive to lift this additional weight off clients’ shoulders so they can focus on the underlying causes of their addiction and achieve total healing. The power of our programming is reflected in our data; our counseling and robust wellness offerings have been proven to be effective in improving mental health outcomes for our clients.
It is essential that co-occurring mental health issues are addressed simultaneously when treating addiction. Upon admission to our program, clients undergo a thorough initial assessment to monitor their mental health, including the existence of depression and anxiety symptoms, substance cravings, difficulty remaining focused, and any challenges falling asleep. During their treatment stay, clients participate in activities and programs focused on improving these areas. At the end of their stay, readings are taken to monitor changes in these five key areas, and the results show:
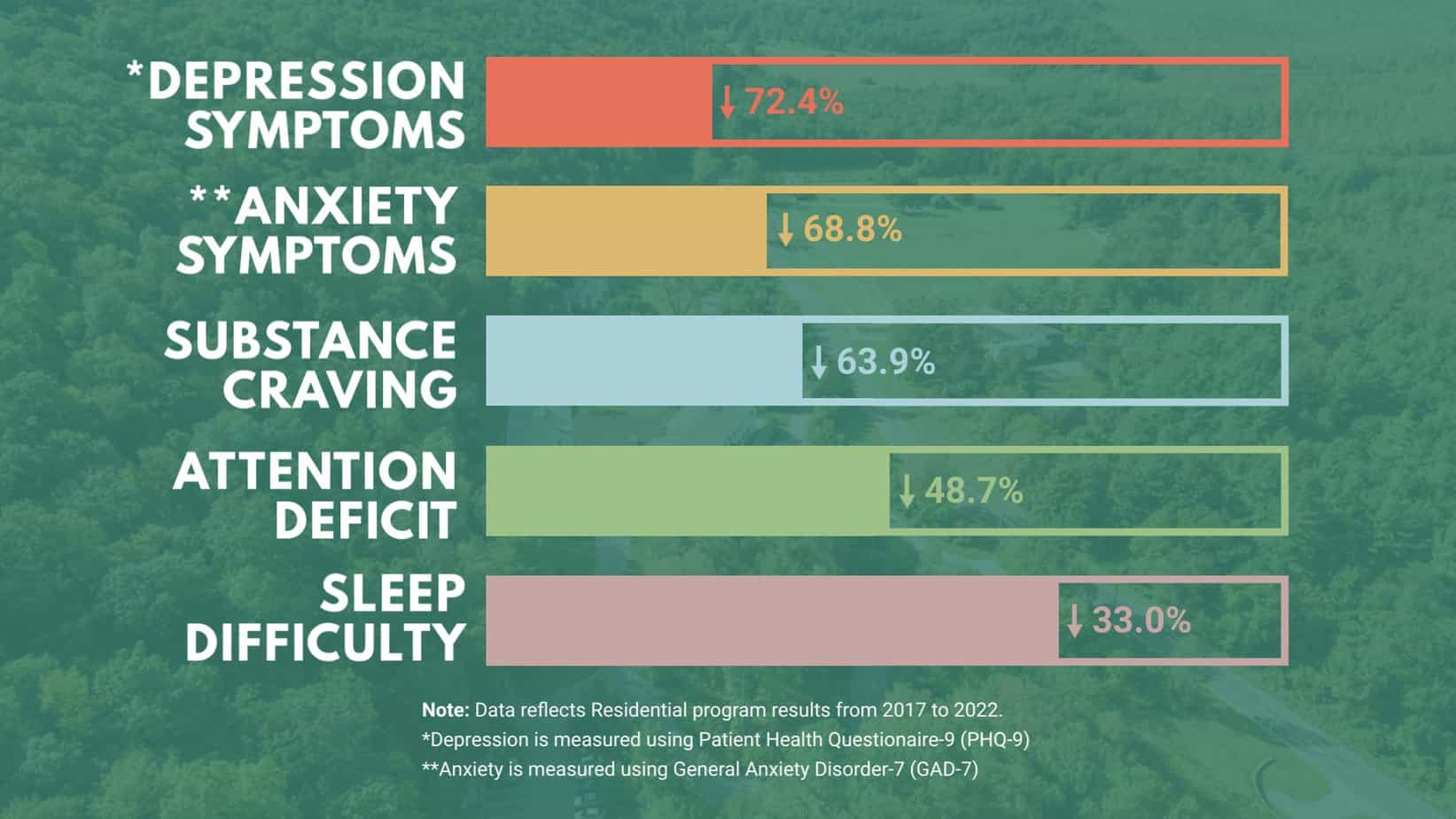
What Do These Mental Health Improvements Mean for Clients’ Recovery from Addiction?
Depression and Anxiety
While it is normal to experience some level of day-to-day stress, an excessive amount of worry, anxiety and sadness can lead to and/or compound physical and mental health disorders. Among our clients, approximately 72.6 percent were clinically diagnosed with anxiety upon entering treatment and 58.1 percent were diagnosed with depression.
From the very beginning of treatment, Mountainside provides programming to help each client improve in critical areas of emotional well-being. In addition to daily group counseling, each client participates in three weekly individual psychotherapy sessions with a therapist to address their unique triggers and explore healthier means of coping with mental health concerns. We are happy to report that upon completion of our Residential program, clients showed a 72.4 percent reduction in depression symptoms and a 68.8 percent decrease in anxiety symptoms.
Substance Cravings
The importance of decreased substance cravings for those struggling with addiction is clear. The fewer drug and alcohol cravings a person experiences, the lower their risk of recurrence and the higher their chances of long-lasting recovery. Fewer substance cravings mean that individuals can channel more energy into developing stress coping techniques and strengthening the sober skills they acquire during treatment.
Substance cravings can be debilitating, especially for those in early recovery. Mountainside’s team checks in on clients’ cravings and adjusts their wellness plans as needed. For example, wellness practices such as acupuncture – which has proven especially valuable for those struggling with cravings – may be incorporated into clients’ weekly schedules depending on their needs. From start to finish, clients in our Residential program reported a 63.9 percent decrease in substance cravings.
Attention Deficit
Individuals with Attention Deficit Hyperactivity Disorder (ADHD) have been shown to have a greater propensity for substance use disorder (SUD). The Journal of Alcohol and Alcoholism notes “One in three young adults with ADHD had a lifetime alcohol use disorder (36%) compared to 19% of those without ADHD.” Those young adults also had higher rates of cannabis and other drug use disorders. At Mountainside, 22.3 percent of clients present with ADHD at admission. The Substance Abuse and Mental Health Services Administration (SAMHSA) shares that there are commonalities between ADHD and SUD, including “restlessness, emotional dysregulation, and impulsivity.” Whether a client has or does not have ADHD, it is important to remedy problematic behaviors that can stymy healing. Our integrative treatment approach includes holistic practices, like meditation, to help clients sharpen focus, strengthen concentration, and better regulate their feelings—fundamental skills necessary for recovery success. Mountainside’s Residential clients saw a 48.7 percent decrease in attention deficit symptoms upon discharge.
Sleep Habits
The many benefits of a good night’s sleep have been well-documented. They include a stronger immune system, heightened productivity, improved mood, and lower stress levels. Sleep hygiene is even more crucial for those struggling with substance use and mental health disorders. There is a close link between sleeping difficulties and substance use. Using drugs and alcohol can lead to trouble sleeping, while insufficient sleep can raise a person’s risk of relapse, according to the journal Sleep Medicine Reviews.
Through evaluation by our medical team and participation in healthy living workshops, individuals acquire sleep education and implement what they have learned. We found that after completing Residential treatment, clients had 33.0 percent less difficulty sleeping on average compared to their first five days of treatment.
The Bottom Line
While issues such as depression and anxiety do not disappear overnight, Mountainside clients have made significant strides in these areas within a short period of time because of their stay in treatment. With the guidance of our expert team, individuals can acquire the necessary tools to address substance cravings and attention deficit, improve their sleep and find the space to focus on addressing their substance use disorder. These tools create a solid foundation for clients to live a happy and healthy life, and achieve long-lasting sobriety.



